Guidelines for the Treatment of Adults with Metastatic Brain Tumors
7. The Role of Steroids in the Treatment of Adults with Metastatic Brain Tumors
Download PDF Neurosurgery, 2019
Sponsored by: The Congress of Neurological Surgeons and the Section on Tumors
Affirmation of Educational Benefit by: The Congress of Neurological Surgeons and the American Association of Neurological Surgeons
Timothy C. Ryken, MD, MS,1 John S. Kuo, MD, PhD,2 Roshan S. Prabhu, MD, MS,3 Jonathan H. Sherman, MD,4 Steven N. Kalkanis, MD,5 Jeffrey J. Olson, MD6
- Section of Neurosurgery, Dartmouth-Hitchcock Medical Center, Lebanon, New Hampshire
- Department of Neurosurgery and Mulva Clinic for the Neurosciences, Dell Medical School, University of Texas at Austin, Austin, Texas
- Southeast Radiation Oncology Group, Levine Cancer Institute, Carolinas Healthcare System, Charlotte, North Carolina
- Department of Neurosurgery, The George Washington University, Washington, DC
- Department of Neurosurgery, Henry Ford Health System, Detroit, Michigan
- Department of Neurosurgery, Emory University School of Medicine, Atlanta, Georgia
Correspondence:
Timothy C. Ryken, MD, MS
Section of Neurosurgery
Dartmouth-Hitchcock Medical Center
One Medical Center Drive
Lebanon, NH 03756
Email: rykent@me.com
Disclaimer of Liability
This clinical systematic review and evidence-based guideline was developed by a multidisciplinary physician volunteer task force and serves as an educational tool designed to provide an accurate review of the subject matter covered. These guidelines are disseminated with the understanding that the recommendations by the authors and consultants who have collaborated in their development are not meant to replace the individualized care and treatment advice from a patient's physician(s). If medical advice or assistance is required, the services of a competent physician should be sought. The proposals contained in these guidelines may not be suitable for use in all circumstances. The choice to implement any particular recommendation contained in these guidelines must be made by a managing physician in light of the situation in each particular patient and on the basis of existing resources.
Keywords:
Brain metastases, cerebral metastases, corticosteroids, neurologic symptoms, practice guideline, steroid dosage, systematic review
ABSTRACT
Questions:
Do steroids improve neurologic symptoms and/or quality of life in patients with metastatic brain tumors compared to supportive care only or other treatment options?
If steroids are given, what dose should be used?
Target population: These recommendations apply to adults diagnosed with brain metastases.
Recommendations
Steroid therapy versus no steroid therapy
Asymptomatic brain metastases patients without mass effect
Insufficient evidence exists to make a treatment recommendation for this clinical scenario.
Brain metastases patients with mild symptoms related to mass effect
Level 3: Corticosteroids are recommended to provide temporary symptomatic relief of symptoms related to increased intracranial pressure and edema secondary to brain metastases. It is recommended for patients who are symptomatic from metastatic disease to the brain that a starting dose of 4–8 mg/day of dexamethasone be considered.
Brain metastases patients with moderate to severe symptoms related to mass effect
Level 3: Corticosteroids are recommended to provide temporary symptomatic relief of symptoms related to increased intracranial pressure and edema secondary to brain metastases. If patients exhibit severe symptoms consistent with increased intracranial pressure, it is recommended that higher doses such as 16 mg/day or more be considered.
Choice of Steroid
Level 3: If corticosteroids are given, dexamethasone is the best drug choice given the available evidence.
Duration of Corticosteroid Administration
Level 3: Corticosteroids, if given, should be tapered as rapidly as possible but no faster than clinically tolerated, based upon an individualized treatment regimen and a full understanding of the long-term sequelae of corticosteroid therapy.
Given the very limited number of studies (two) which met the eligibility criteria for the systematic review, these are the only recommendations that can be offered based on this methodology. Please see “Discussion” and “Summary” section for additional details.
INTRODUCTION
Rationale
Steroids have been used to assist in controlling peritumoral intracerebral edema in the care of patients with newly diagnosed metastatic brain disease.1-12 Dexamethasone has been the steroid most commonly used due to its minimal mineralocorticoid effect. Steroids have been used for palliative care, and, in combination with surgery and radiation, to reduce treatment-related toxicity. Historically, the majority of patients treated with an initial dose of 4 to 8 mg/day responded within 24 to 72 hours. 13 Toxicity and side effects from steroids occur frequently and contribute to the overall morbidity and mortality in this often-tenuous patient population. However, as previously described, a review of the literature continues to demonstrate a lack of well-controlled studies addressing this topic and significant variability in the dosing and administration of steroids in both the symptomatic and asymptomatic patient. 11
Objectives
This updated systematic review addresses the role of corticosteroids in the treatment of metastatic brain disease with the following overall objectives:
1. To systematically review and update the evidence available addressing the use of corticosteroids in the management of patients with brain metastases since the previous review of 2010, 11 again addressing the following questions:
· Do steroids improve neurologic symptoms in patients with metastatic brain tumors compared to no treatment?
· If steroids are given, what dose should be used?
2. To make recommendations based on this evidence for the role of corticosteroids in the management of these patients.
METHODS
Writing Group and Question Establishment
The writers represent a multi-disciplinary panel of clinical experts encompassing neurosurgery and radiation oncology. Together, they were recruited to develop these evidence-based practice guidelines for surgery for metastatic brain tumors. Questions were developed by group consensus recognizing the questions used in the prior guidelines published on this topic and taking into account current salient concerns over the use of steroids in metastatic brain tumor management.
Search Method
The PubMed online database was searched for the period of October 1, 2008 through December 31, 2015, using the following queries in all fields: steroids and brain metastases, and dexamethasone and brain metastases. The results from each search were downloaded into an Endnote library. The libraries were merged and duplicate entries were eliminated. This inclusive search strategy was designed to capture all manuscripts pertaining to brain metastases and steroids for manual review and to determine if any more recent articles had been missed in the prior update. The reference lists of the most relevant and most recent articles were also reviewed, and additional articles selected for initial review.
Study Selection and Eligibility Criteria:
The following inclusion criteria were used for manual review of studies:
1. Published in English with a publication date prior to December 31, 2015.
2. Included only patients with brain metastases.
3. Published in a peer-reviewed journal with comparative data pertaining to the use of steroids in patients with brain metastases.
The search strategy was purposefully as broad as possible given the limited number of relevant articles found in the previous guideline.
Data Collection Process
The initial screening and evaluation of the initial search-returned citations using pre-determined criteria for relevance (initial screen via title/abstract, with a secondary full-text review of potentially relevant manuscripts) was performed by the primary author with additional input from the author group. Data from studies meeting eligibility criteria was then extracted by a single reviewer and checked by a minimum of two additional reviewers.
Assessment for Risk of Bias
Studies selected for full-text review were evaluated, in addition to the overall quality of the study design, for specific issues of bias. Particular attention was paid to potential bias related to selective case choice and reporting, publication bias, bias related to change in treatment methods over time, hidden agenda bias when perceived, and variability due to inconsistencies in data entry and oversight. When encountered concerns about specific examples of bias in the published data were noted in the evidentiary tables. The class of data and subsequent level of recommendation was then adjusted accordingly.
Description of the Data Classification System and Recommendation Formulation
The quality of each study regarding metastases-specific data and the strength of the recommendations within this work were graded according to the American Association of Neurological Surgeons (AANS)/Congress of Neurological Surgeons (CNS) criteria ( here ).
RESULTS
Study Selection and Characteristics
In the 2010 guideline, 11 despite the widespread use of steroids in the management of brain metastases, only 2 publications met the stated eligibility criteria. 13 , 14 Given the limited data yielded by the literature search, additional searches were undertaken by reviewing the bibliographies of relevant recent publications and additional review of any relevant published literature addressing the treatment of metastatic brain disease for references to steroid administration. These articles are summarized in the discussion below. The publications that report the Quality of Life after Treatment for Brain Metastases (QUARTZ) trial 1 , 8,12, 15 were summarized in the publication by Mulvenna et al 1 , 12 in 2016. Mulvenna et al 12 was published after the literature review for this guideline was performed, but is referenced for completeness, even though it was not included as evidence to support the recommendations of this guideline update.
Results of Individual Studies, Discussion of Study Limitations, and Risk of Bias
All of the following studies were graded as Class 3 evidence. Two studies were included in the original 2010 guideline.11 Vecht et al 13 conducted a randomized study of 4, 8, and 16 mg/day dosing of dexamethasone and demonstrated no advantage to higher dosing in patients without symptomatic intracranial hypertension. Two consecutive double-blind randomized trials in patients with brain metastases and Karnofsky performance scores (KPS) <80 were designed to evaluate the minimum effective dose of oral dexamethasone. Initially, a dexamethasone dosage of 8 mg/day (group 1) was compared to 16 mg/day (group 2), followed by a comparison of 4 mg/day (group 3) versus 16 mg/day (group 4). The outcomes of interest were alteration in KPS and the frequency of side effects at days 0, 7, 28, and 56.
Both groups showed improvement, but there was no significant difference in KPS improvement comparing the 8-mg group versus the 16-mg group at day 7 (mean 8.0 ± 10.1 versus 7.3 ± 14.2).
In the second trial conducted by Vecht et al 13, both groups showed improvement. There was no significant difference between the 4 mg and 16 mg groups, comparing 6.7 ± 11.3 points at day 7 and 7.1 ± 18.2 points at day 28 versus 9.1 ± 12.4 and 5.6 ± 18.5 points, respectively. Side effects were more frequent in the 16 mg/day versus the 4 mg/day group at day 28 (combined frequency 91% versus 46%, p<.03).
The authors concluded that the lower doses of 4 and 8 mg dexamethasone per day had an equivalent effect on improving neurologic performance when compared with a dose of 16 mg/day at 1 and 4 weeks of treatment, in moderately symptomatic patients without signs of impending herniation. The dosing recommendation from this study was 4 mg/day dosage with a dose taper for 28 days in patients with no symptoms of mass effect.
Wolfson et al 14 randomized 12 patients undergoing whole brain radiation therapy following an initial dose of 24 mg dexamathasone into a group receiving 4 mg every 6 hours during the radiotherapy versus no additional steroids. Although more patients were improved in the steroid group (29% versus 0%), the small size and complete lack of statistical analysis resulted in this study being excluded as evidence in the previous report.
Given the extremely limited number of studies that satisfied the conditions of inclusion, an additional discussion of published literature on the subject of corticosteroids in metastatic brain disease is provided to offer a larger context for this topic. While the following studies were not part of the body of evidence considered in formulating treatment recommendations in this evidence-based guideline, they do highlight areas of interest where clinical trials are still required to answer important steroid-related questions.
A series of authors have published contemporary updates, reviews, and consensus documents that recommend steroid therapy in the management of CNS metastatic disease, with no additional data provided. 3 , 4, 7 , 9,10, 15-18 For example the systematic review by Tsao et al provides little data on how the actual review was conducted. 9
The series of articles published describing the QUARTZ study compare palliative whole brain radiation therapy versus supportive care with steroids, and are significant in that they appear to establish the role of steroids as a baseline of care for the symptomatic patient with central nervous system metastasis. 1 , 8,12, 15 This study provides randomized data on the comparison of whole brain radiotherapy versus steroids alone but provides no comparative data on dosing or the comparison of no steroid versus steroid. It appears that this issue has been assumed to be adequately addressed with clinical practice, because no comparative studies addressing this issue have appeared in >20 years.
Although they do not provide comparative data, several additional studies are noted as they include issues related to steroid use in this population. Not mentioned in the 2010 guideline, 11 Sturdza et al19 studied steroid prescribing practices and patient side effects in 88 patients identified in the Palliative Radiation Oncology database. Forty-five percent of physicians used a dexamethasone dose of 4 mg 4 times daily (16mg/day) with 60% using a 4-week taper. The most common side effects were increased appetite or weight gain (46%), insomnia (24%), gastrointestinal symptoms (20%), and proximal muscle weakness (28%). The authors concluded that considerable variation in the prescribing practices existed even within a single institution, with many patients receiving high doses of steroids for considerable periods of time and developing related side effects, and they propose a prospective study to standardize dosing and taper practices to optimize management and minimize toxicity.
Pulenzas et al 6 surveyed a cohort of patients undergoing whole brain radiation therapy for changes in fatigue scores using a broad panel of outcome measures, including the Edmonton Symptom Assessment System, the Brain Symptom and Impact Questionnaire, the Spitzer Questionnaire, the European Organization for Research and Treatment of Cancer (EORTC) Quality of Life Questionnaire, the EORTC brain module, the EORTC Quality of Life Questionnaire Core 15 Palliative, and the Functional Assessment of Cancer Therapy-General. The authors concluded that fatigue was significantly increased and quality of life significantly reduced over the first month in all patients. Increased fatigue was significantly related with decreased overall QOL. Interestingly, for all groups, there was no significant difference in fatigue scores or quality of life with or without the addition of dexamethasone.
Alan et al5 studied the impact of preoperative steroids on 30-day morbidity and mortality of >4000 patients undergoing craniotomy for resection of malignant brain tumors (metastatic brain tumors 37.5% (n = 1611) and primary malignant gliomas 62.5% (n = 2796). Approximately 23% of patients received perioperative steroids (n = 1009). Logistic regression was used to assess the association between preoperative steroid use and perioperative complications before and after 1:1 propensity score matching. In the unmatched cohort (n = 1009), steroid use was associated with decreased length of hospitalization (odds ratio 0.7; 95% confidence interval 0.6-0.8). In this same group, the incidence of readmission (odds ratio 1.5; 95% confidence interval 1.2-1.8) was increased. In the matched cohort (n = 465), steroid use was not statistically associated with any adverse outcomes. As an independent risk factor, preoperative steroid use was not associated with any observed perioperative complications.
The authors concluded that preoperative steroids do not independently compromise the short-term outcome of craniotomy for resection of malignant brain tumors. Separating out the metastatic versus the primary tumor patients is difficult from the data presented and limits the ability to formulate recommendations.
Synthesis of Results
Vecht et al13 continues to provide the most convincing data on the role for steroids in patients with brain metastases and for the choice of dosing. Based on their observations of improvement in all groups treated with steroids, Level 3 recommendations were made in the 2010 Guideline. 11 The results of this guideline confirms the validity of those recommendations, because no novel evidence has been published on this topic since 2010.
Given the very limited number of studies only two of which met the eligibility criteria for the systematic review, these are the only recommendations that can be offered based on this methodology. Please see the Discussion section for additional details.
DISCUSSION
Although comparative studies addressing various steroid dosing regimens are generally lacking, studies addressing additional topics of interest have been published in recent years. 1 , 2,5,6, 12 A better understanding of the toxicity related to routine steroid use continues to develop, and this research would support the principle of using the lowest effective steroid dose. 6 , 19 The design of large clinical trials in which a steroid treatment-only groups are considered the “best supportive care” group underlines the conviction most physicians hold for the critical role of steroids in managing the patient with symptomatic central nervous system metastatic disease. 1 , 8, 15
The issue of dosing regimen is problematic to address based on the evidence available. The study noted by Vecht et al 13 used only 4 times daily dosing and does not address alternative dosing regimens. Therefore, only recommendations on total amount per day have been formulated. It is recognized as common practice that alternative dosing, such as twice daily, is acceptable practice.
In addition, the ability of steroids to reduce the likelihood of treatment-related toxicity, either following surgery or radiotherapy, continues to be of interest and warrants additional study at least as a component of the data collection process in clinical trials. 3 , 5
CONCLUSION AND KEY ISSUES FOR FUTURE INVESTIGATIONS
It is clear from this review of the literature that steroids are a mainstay of treatment for patients with metastatic brain disease despite the relative lack of high-quality evidence supporting any specific therapy. Based on the literature available for this guideline update, larger prospective or carefully planned retrospective studies should be considered to clarify more specific patient-dependent dosing. Complications related to steroid use, including adrenal insufficiency with tapering, should continue to be monitored, and perhaps alternative approaches to reducing peritumoral edema could be explored to eliminate the unwanted but common side effects of steroid therapy entirely.
Potential Conflicts of Interest
The Brain Metastases Guideline Update Task Force members were required to report all possible conflicts of interest (COIs) prior to beginning work on the guideline, using the COI disclosure form of the AANS/CNS Joint Guidelines Review Committee, including potential COIs that are unrelated to the topic of the guideline. The CNS Guidelines Committee and Guideline Task Force Chair reviewed the disclosures and either approved or disapproved the nomination. The CNS Guidelines Committee and Guideline Task Force Chair are given latitude to approve nominations of task force members with possible conflicts and address this by restricting the writing and reviewing privileges of that person to topics unrelated to the possible COIs. The conflict of interest findings are provided in detail in the companion introduction and methods manuscript (here).
Disclosures
These evidence-based clinical practice guidelines were funded exclusively by the Congress of Neurological Surgeons and the Tumor Section of the Congress of Neurological Surgeons and the American Association of Neurological Surgeons, which received no funding from outside commercial sources to support the development of this document.
ACKNOWLEDGEMENTS
The authors acknowledge the CNS Guidelines Committee for its contributions throughout the development of the guideline and the AANS/CNS Joint Guidelines Review Committee for its review, comments, and suggestions throughout peer review, as well as Trish Rehring, MPH, CHES, CNS Guidelines Senior Manager, and Mary Bodach, MLIS, Senior Guidelines Specialist, for their assistance. Throughout the review process, the reviewers and authors were blinded from one another. At this time, the guidelines task force would like to acknowledge the following individual peer reviewers for their contributions: Manish Aghi, MD, PhD, Manmeet Ahuwalia, MD, Sepideh Amin-Hanjani, MD, Edward Avila, MD, Maya Babu, MD, MBA, Kimon Bekelis, MD, Priscilla Brastianos, MD, Paul Brown, MD, Andrew Carlson, MD, MS, Justin Jordan, MD, Terrence Julien, MD, Cathy Mazzola, MD, Adair Prall, MD, Shayna Rich, MD, PhD, Arjun Sahgal, MD, Erik Sulman, MD, May Tsao, MD, Michael Voglebaum, MD, Stephanie Weiss, MD, and Mateo Ziu, MD.
Figure 1. PRISMA Flowchart
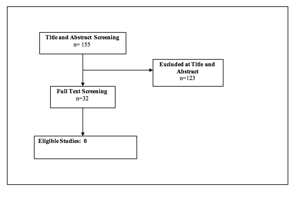
REFERENCES
1. Mulvenna P, Nankivell M, Barton R, et al. Dexamethasone and supportive care with or without whole brain radiotherapy in treating patients with non-small cell lung cancer with brain metastases unsuitable for resection or stereotactic radiotherapy (QUARTZ): results from a phase 3, non-inferiority, randomised trial. Lancet. Sep 2 2016.
2. Agar M, Koh ES, Gibbs E, et al. Validating self-report and proxy reports of the Dexamethasone Symptom Questionnaire -Chronic for the evaluation of longer-term corticosteroid toxicity. Support Care Cancer. Mar 2016;24(3):1209-1218.
3. Tsao MN. Brain metastases: advances over the decades. Ann Palliat Med. Oct 2015;4(4):225-232.
4. Pruitt AA. Medical management of patients with brain tumors. Continuum (Minneap Minn). Apr 2015;21(2 Neuro-oncology):314-331.
5. Alan N, Seicean A, Seicean S, Neuhauser D, Benzel EC, Weil RJ. Preoperative steroid use and the incidence of perioperative complications in patients undergoing craniotomy for definitive resection of a malignant brain tumor. J Clin Neurosci. Sep 2015;22(9):1413-1419.
6. Pulenzas N, Khan L, Tsao M, et al. Fatigue scores in patients with brain metastases receiving whole brain radiotherapy. Support Care Cancer. Jul 2014;22(7):1757-1763.
7. Expert Panel on Radiation Oncology-Brain M, Lo SS, Gore EM, et al. ACR Appropriateness Criteria(R) pre-irradiation evaluation and management of brain metastases. J Palliat Med. Aug 2014;17(8):880-886.
8. Langley RE, Stephens RJ, Nankivell M, et al. Interim data from the Medical Research Council QUARTZ Trial: does whole brain radiotherapy affect the survival and quality of life of patients with brain metastases from non-small cell lung cancer? Clin Oncol (R Coll Radiol). Mar 2013;25(3):e23-30.
9. Tsao MN, Khuntia D, Mehta MP. Brain metastases: what's new with an old problem? Curr Opin Support Palliat Care. Mar 2012;6(1):85-90.
10. Pruitt AA. Medical management of patients with brain tumors. Curr Treat Options Neurol. Aug 2011;13(4):413-426.
11. Ryken TC, McDermott M, Robinson PD, et al. The role of steroids in the management of brain metastases: a systematic review and evidence-based clinical practice guideline. J Neurooncol. Jan 2010;96(1):103-114.
12. Mulvenna P, Nankivell M, Barton R, et al. Dexamethasone and supportive care with or without whole brain radiotherapy in treating patients with non-small cell lung cancer with brain metastases unsuitable for resection or stereotactic radiotherapy (QUARTZ): results from a phase 3, non-inferiority, randomised trial. Lancet. Oct 22 2016;388(10055):2004-2014.
13. Vecht CJ, Hovestadt A, Verbiest HB, van Vliet JJ, van Putten WL. Dose-effect relationship of dexamethasone on Karnofsky performance in metastatic brain tumors: a randomized study of doses of 4, 8, and 16 mg per day. Neurology. Apr 1994;44(4):675-680.
14. Wolfson AH, Snodgrass SM, Schwade JG, et al. The role of steroids in the management of metastatic carcinoma to the brain. A pilot prospective trial. Am J Clin Oncol. Jun 1994;17(3):234-238.
15. Mulvenna PM. The management of brain metastases in patients with non-small cell lung cancer-is it time to go back to the drawing board? Clin Oncol (R Coll Radiol). Jun 2010;22(5):365-373.
16. Roth P, Wick W, Weller M. Steroids in neurooncology: actions, indications, side-effects. Curr Opin Neurol. Dec 2010;23(6):597-602.
17. Nguyen TD, DeAngelis LM. Brain metastases. Neurol Clin. Nov 2007;25(4):1173-1192, x-xi.
18. Soffietti R, Cornu P, Delattre JY, et al. EFNS Guidelines on diagnosis and treatment of brain metastases: report of an EFNS Task Force. Eur J Neurol. Jul 2006;13(7):674-681.
19. Sturdza A, Millar BA, Bana N, et al. The use and toxicity of steroids in the management of patients with brain metastases. Support Care Cancer. Sep 2008;16(9):1041-1048.
Source: Neurosurgery, January 9, 2019